In our previous article, we explained what Nipah virus is and why it commands global attention despite being rare. Since then, health authorities across Asia have intensified surveillance not because the virus is spreading widely, but because early action prevents escalation. The current situation illustrates a region applying hard-earned pandemic lessons with speed and precision.
Current Status: A Small Cluster Under Tight Control
As of January 28, 2026, the outbreak remains limited to West Bengal, India, with two laboratory-confirmed cases. Both patients are healthcare workers infected in a nosocomial (hospital acquired) setting after exposure to an undiagnosed patient with severe respiratory illness.
Extensive contact tracing has identified 196 close contacts, all of whom have tested negative and remain symptom free.
Earlier media reports mentioned higher numbers, but on January 27, India’s Ministry of Health and Family Welfare, alongside the National Centre for Disease Control (NCDC), issued a formal clarification urging the public to disregard “speculative figures.” The official count remains two confirmed cases, reinforcing that the situation is contained and under active monitoring.
No other country has reported an imported infection.
Why West Bengal Matters After 19 Years
West Bengal has not recorded Nipah cases in nearly two decades. Scientists are now examining whether environmental changes, habitat disruption, or shifts in fruit bat migration patterns may be influencing the virus’s reappearance in a region previously considered low risk. This does not indicate widespread spread but it highlights how zoonotic diseases can re-emerge when ecological balances change.
Regional Response: Preparedness Without Panic
Countries across Asia have activated precautionary protocols:
Thailand
Since the weekend, authorities have screened about 1,700 passengers arriving from West Bengal at major airports. Thermal cameras, health declaration forms, and symptom monitoring are in place. Public Health Minister Phatthana Phromphat confirmed that no infections have been detected in Thailand, emphasizing that screenings are preventive.
Nepal
Health desks are active at Tribhuvan International Airport and major land crossings, with isolation facilities prepared in Koshi Province.
Taiwan
Officials are considering listing Nipah as a Category 5 disease, enabling mandatory reporting and rapid state control. A travel advisory urges avoidance of raw date palm sap and unwashed fruit.
Hong Kong
Authorities rate the risk as low but maintain gate temperature checks as a precautionary safeguard.
These steps reflect vigilance, not evidence of widespread transmission.
Understanding the Real Risk
Nipah’s reputation comes from its severity, not its ease of spread.
- Transmission: Requires close contact with respiratory droplets or bodily fluids, or consumption of contaminated food. It is not considered truly airborne like COVID-19.
- Contagiousness: The virus generally has an R₀ below 1, meaning outbreaks tend to fizzle out rather than expand exponentially.
- Incubation Period: While rare cases may incubate for up to 45 days, the vast majority of infections appear within 4–14 days.
- Severity: It can rapidly progress from flu-like illness to encephalitis (brain inflammation), which drives its high fatality rate (40–75%).
These factors explain why hospitals are on high alert, yet the general public outside exposure settings faces low risk.
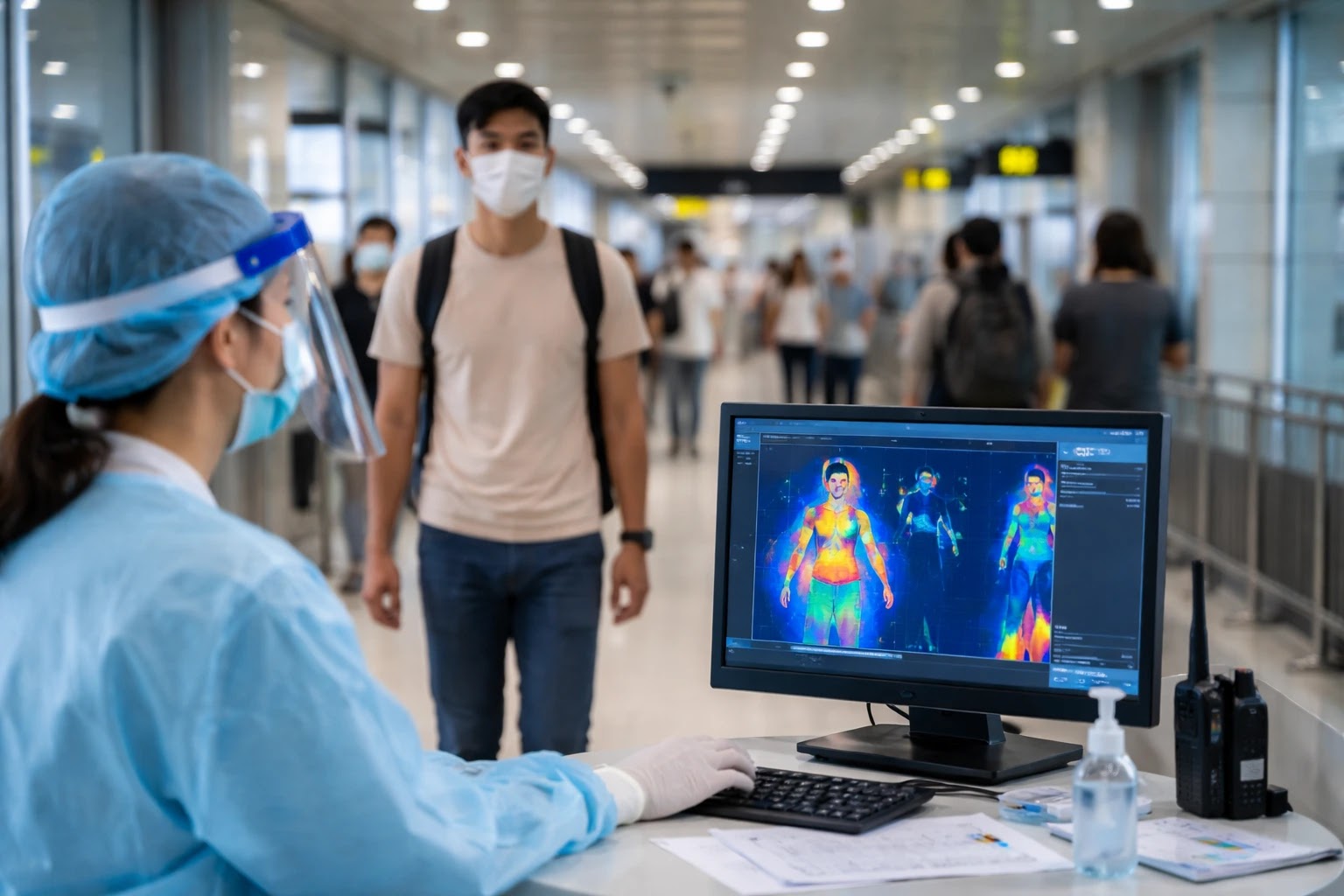
Airport Screenings: What They Actually Do
Travel screenings involve:
- Thermal imaging to detect fever (≥38°C / 100.4°F)
- Health “beware” cards and self-monitoring portals
- Staff trained to identify symptom progression from fever and headache to confusion or breathing distress
Because someone in the incubation phase may have no fever, these measures don’t catch every case. Instead, they reduce the chance of unnoticed spread.
Scientific Progress: A Shift From Past Outbreaks
Unlike previous Nipah outbreaks, preparedness tools now exist:
- Vaccine Development: The University of Oxford is leading a Phase II trial of the ChAdOx1 NipahB vaccine, while the Serum Institute of India serves as the manufacturing partner and maintains an investigational reserve of up to 100,000 doses for emergency use if needed.
- Experimental Therapies: Monoclonal antibodies and some repurposed antivirals are being used under controlled or compassionate use frameworks in intensive care settings.
These are not yet public solutions but represent a major advance in outbreak readiness.
WHO Position: Moderate Global Risk
The World Health Organization classifies the situation as moderate risk globally, emphasizing containment, surveillance, and infection control guidance rather than travel restrictions.
Nipah remains on the WHO’s priority pathogen list due to its lethality and lack of licensed countermeasures.
Bottom Line
- Only two confirmed cases, both hospital-linked
- No community spread detected
- International screenings are preventive
- Public risk remains low outside close-contact exposure
- Preparedness and awareness are the region’s strongest defenses
The story in 2026 is not one of uncontrolled spread, it is one of early detection, coordinated response, and scientific progress working together to prevent a crisis.